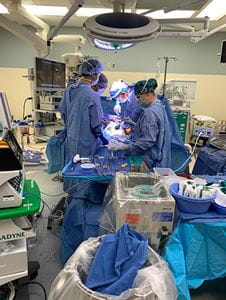
Chronic Pancreatitis is an inflammation of the pancreas that does not heal or improve—it gets worse over time and leads to permanent damage. This disease can eventually impair a patient's ability to digest food and make pancreatic hormones. Most individuals with Chronic Pancreatitis experience upper abdominal pain, although some have no pain at all. The pain may spread to the back, worsen with eating or drinking, and become constant and disabling.
According to research review by Nicholas J. Zyromski, M.D. Professor of Surgery and Thomas K. Maatman, M.D General Surgery Resident, Chronic Pancreatitis in the US is diagnosed with increasing frequency and costs more than $150 million annually to treat.
However, the IU Heath Network now offers an operation called total pancreatectomy and islet autotransplantation an operation that was introduce in the 1970s that could offer more options for patients suffering from chronic pancreatitis.
Evan L. Fogel, MD, an IU Professor of Medicine, explained that a total pancreatectomy and islet autotransplantation is done in two parts. First is the removal of the pancreas, and second, the auto islets are removed from the pancreas and transplanted to the liver. The pancreatectomy relieves pain while the auto islet transplantation reduces the need for insulin, which would otherwise be necessary for people without a pancreas.
Currently, IU has one of the highest volumes of pancreas operations in the nation.
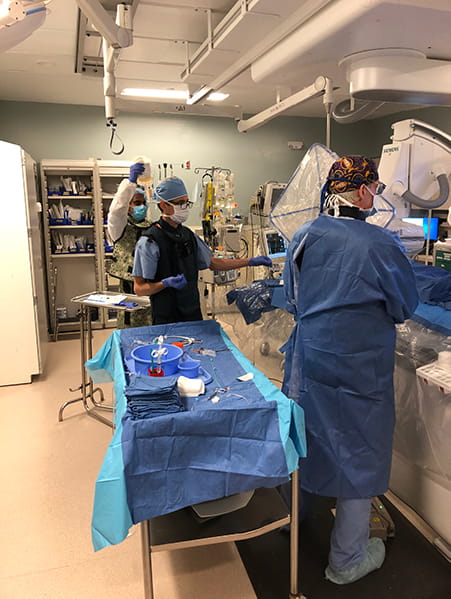 “We do Between 300 and 350 pancreatic operations at University Hospital every year or two,” said Zyromski. “We are number two, in terms of pancreas surgery volume, in the country.”
“We do Between 300 and 350 pancreatic operations at University Hospital every year or two,” said Zyromski. “We are number two, in terms of pancreas surgery volume, in the country.”
This procedure will give those that need a pancreas removal a chance to live better glucose control. With the standard method, a total pancreatectomy will cause diabetes in the patient.
“If the surgeon removes the pancreas, the patient will develop diabetes 100 percent of the time,” explained Fogel. “So, to try and prevent that, that's where the second part of the surgery comes in, the islet autotransplantation.”
Fogel explained that islet are the cells in the pancreas that make insulin. The hope for this surgery is that a surgeon can remove the pancreas islet cells and introduce them back into the body to continue producing insulin. They infuse the islet cells into the liver’s portal vein in an attempt to maintain the same secretion of insulin and a chance to live with better glucose control for patient.
Pancreatitis can be such a complex disease that many medical specialties are involved in the treatment and management. Zyromski explained how the complexity of chronic pancreatitis may require an extensive team to help with patient care including a gastroenterologist, an endocrinology team, gastrointestinal psychologist, nutritionist, pancreatitis nurse coordinator, general surgeons, pain management specialist, and radiologist. As many as half a dozen departments may be represented in one case. This program will now allow for a more comprehensive education for residents at the IU School of Medicine.
“Managing complex diseases like Chronic Pancreatitis is educational on a number of different levels,” said Zyromski. “I think some of the greatest benefits of the educational piece for the residents to understand are the human physiology and understanding how to work in a multidisciplinary team, which is obviously necessary for a complex disease like this from the technical side.”
With this department offering such an innovative procedure, it will only improve the quality of life of Indiana pancreatitis patients. “We have a strong and really well-established, pancreatitis program and the total pancreatectomy and islet autotransplantation will be an additional piece to our very well established, multidisciplinary program,” said Zyromski. “This new addition will really help round out the program and it’s a very nice addition to a solid program.”