The most common pediatric cardiac defects continue to be congenital heart disease, which affect nearly one percent of all newborns. Defects that previously were considered hopeless are now successfully repaired or palliated. Today, more patients with congenital heart disease are over the age of 18 than under 18 years of age.
Clinical Focus Areas
The congenital heart program spans prenatal diagnosis, pediatric congenital disease and the adult congenital heart disease continuum. The division provides clinical care covering a broad spectrum services.
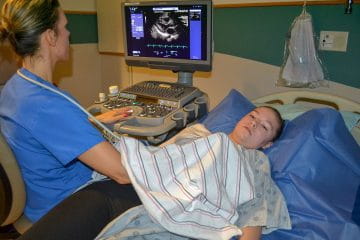
Echocardiography
One of the most useful diagnostic modalities for assessing congenital heart defects is the echocardiogram, which uses noninvasive, high-frequency sound waves to reveal complex cardiac anatomy and physiology. This essential technology has eliminated the need for cardiac catheterization for many defects. IU School of Medicine clinicians at Riley Hospital for Children have additional specialized training and annually perform more than 10,000 pediatric and fetal echocardiograms. Their expertise is widely recognized among other hospitals in the Midwest, which rely on these cardiologists to interpret more than 5,000 echos from their own institutions.
Riley Hospital for Children was the first in Indiana to have a pediatric echo lab accredited by the Intersocietal Accreditation Commission. In addition to traditional echos, IU School of Medicine cardiologists dealing with more complex cases often perform transesophageal echos (TEE) when they need additional views. A transesophageal echo also can guide interventional catheterizations and provide immediate assessment in the operating room.
Echocardiograms are performed throughout Riley Hospital and the Riley Heart Center including the operating room and catheterization lab for intra-operative assessment to guide surgical interventional procedures. The Riley Hospital echo lab was one of the first all-digital laboratories in Indiana. New technologies and systems are applied continuously to ensure that studies can be assessed and reviewed 24 hours a day for patient care.
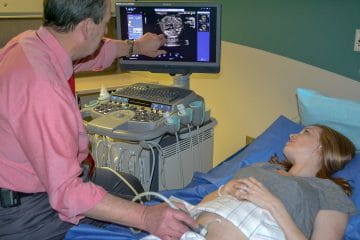
Fetal Echocardiography
Congenital heart defects are the most common birth defects, occurring in approximately one out of every 125 live births. Many of these defects can be identified in utero with specialized fetal echocardiography. This can allow for immediate treatment or counseling and planning that enhances outcomes. The fetal cardiology specialists at IU School of Medicine work closely with maternal-fetal medicine specialists and perform more than 1,400 detailed fetal cardiac ultrasounds at multiple sites, providing immediate consultation and discussion. These pediatric specialists work closely with the referring physicians as well as the surgical, neonatal and other Riley specialists to help formulate the best course of treatment for the individual patient and specific congenital heart defect.

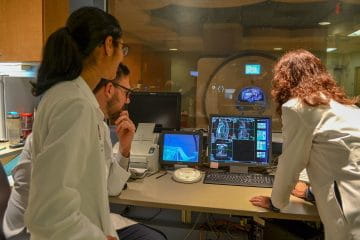
Cardiac Magnetic Resonance (CMR)
The Cardiac Magnetic Resonance (CMR) program at Riley Hospital for Children at IU Health (Indianapolis) is unique in the state of Indiana, providing thorough and in-depth details on cardiac structure and function in children and young adults with all varieties of heart disease. At Riley, IU School of Medicine faculty pediatricians perform highly specialized cardiac magnetic resonance exams on more than 300 patients annually. Cardiac magnetic resonance does not use ionizing radiation and the imaging is not invasive, often providing an alternative to cardiac catheterization. This makes cardiac magnetic resonance a very easy and low-risk procedure for many patients to undergo. Cardiac magnetic resonance can also answer questions that echocardiography may not be able to answer and often plays a critical role in patient care when making decisions and planning for heart surgery or other needed cardiac interventions. The Cardiac Magnetic Resonance Program at Riley is guided by two IU School of Medicine pediatric cardiologists and one pediatric radiologist, the only pediatric physicians in Indiana qualified to perform and interpret cardiac magnetic resonance studies.
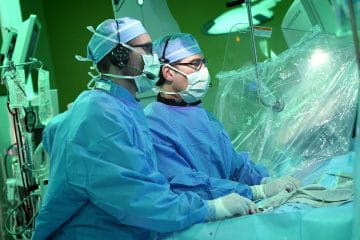
Cardiac Catheterization
Cardiac catheterization, formerly only used for diagnostic purposes to aid in surgical management, has exploded over the last 15-20 years to include numerous methods of treatment without the need for surgery or in collaboration with surgical techniques. Rapidly advancing technology is allowing for the diagnosis of the most complex cardiac defects and therapeutic treatment of a variety of cardiac birth defects is now possible. Some of these defects include atrial septal defect, patent ductus arteriosus, ventricular septal defect, coarctation of the aorta, pulmonary stenosis, and aortic stenosis. Valves have been implanted in the pulmonary and tricuspid positions solely in the cardiac catheterization lab, avoiding the need for surgery altogether. IU School of Medicine interventional pediatric cardiologists at Riley Hospital have been at the forefront of those advancements. Recent advancements have allowed transcatheter closure of patent ductus arteriosus in tiny premature infants, who previously could only undergo surgery. These cardiologists have been among a small group of experts nationwide involved in clinical research trials for Amplatzer Septal and Duct Occluders and Nit-Occlude that treats atrial septal defects (ASD) and patent ductus arteriosus (PDA). Numerous clinical trials of newer medical devices are ongoing.
The cardiac cath labs are located within the Riley Hospital operating room area, across the hall from the Cardiac Surgery OR’s, which greatly facilitates collaboration of the interventional cardiologists and cardiac surgeons. One of the cath labs is designed as a hybrid cath lab suite, allowing both surgeons and cardiologists to work jointly in managing complex heart defects. Combined interventional and surgical techniques (hybrid procedures) have been performed at Riley Hospital for Children since 2004. Examples of such cases have included implantation of PDA stents, pulmonary valve perforation in pulmonary atresia, and ligation of unusual collateral vessels whereby angiographic localization provides immediate feedback before and after surgical intervention.
A team model of care shapes the treatment in the catheterization laboratory and recovery within the Riley Heart Center. Pediatric Interventional cardiologists and cath lab nursing personnel work closely with pediatric cardiac anesthesiologists for all procedures, and intensivists are involved whenever necessary. More than 500 pediatric cardiac catheterizations (diagnostic, interventional, biopsy and electrophysiologic) are performed by IU School of Medicine faculty each year.
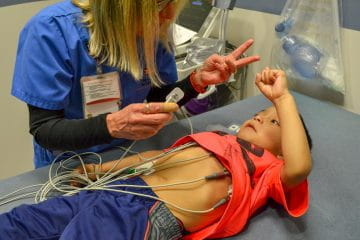
Electrophysiology
The Riley Pediatric Arrhythmia Center provides comprehensive, state-of-the-art, diagnostic and treatment services for patients and families with heart rate and rhythm concerns. In addition to electrocardiogram (EKG), treadmill rhythm evaluation, home EKG monitors, and event monitors, IU School of Medicine faculty at this center offer electrophysiology study with catheter ablation and implantation of pacemakers and cardiac defibrillators (including remote monitoring of these devices throughout the state and region). These physicians partner with colleagues in cardiovascular genetics to provide a joint inherited arrhythmia clinic for the evaluation and treatment of conditions including Long QT syndrome and other potentially life-threatening arrhythmias. Similarly, the center offers a multidisciplinary adult congenital heart disease arrhythmia clinic focused on the needs of this growing community while offering ablation and device treatment of arrhythmias for these patients with complex cardiac anatomy.
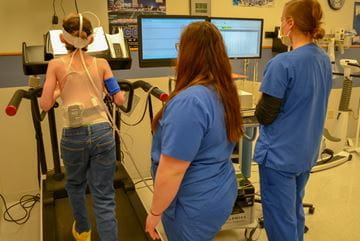
Stress Testing
More than 350 cardiac exercise stress tests take place at Riley Hospital for Children each year in a laboratory dedicated to sophisticated evaluation of the response to maximal exercise. Reasons for exercise stress tests vary from cardiac clearance for school sports to evaluations after fainting episodes, exercise-induced chest pain, abnormal heart rhythms, cardiac surgery or heart transplantation. State-of-the-art equipment used for exercise testing includes treadmills and bicycles with computer-controlled workload adjustments, measurement of peak oxygen consumption, blood oxygen saturation, continuous heart rate and rhythm, blood pressure, and other respiratory and metabolic parameters. The pediatric cardiology team utilizes an exercise physiologist to coordinate exercise stress tests, provides individualized exercise programs for patients, and assists in exercise-related research endeavors.
Adult Congenital Heart Disease Program
As a result of extremely successful diagnostic and treatment strategies developed and employed over the past half century, the number of children surviving to adulthood with congenital heart defects in the United States exceeds one million. Of these, the majority require lifelong care by health care professional with expertise in the care of adult congenital heart disease. Meeting the unique and complex needs of this special population of patients is the mission of IU Health’s Adult Congenital Heart Disease Program, which is jointly staffed by IU School of Medicine pediatric cardiologists and adult congenital cardiologists from IU School of Medicine’s Krannert Institute of Cardiology, as well as the Division of Congenital Cardiac Surgery. This collaborative effort among leading physicians ensures expertise in the wide range of cardiovascular problems facing these patients. Specially trained technicians, sonographers, and nurse clinicians complete the team and provide the breadth of services necessary for optimal health care and physician training. The program sees in excess of 1000 outpatients yearly and provides comprehensive service, including the full range of adult congenital heart surgery, innovative interventional cardiology procedures, advanced arrhythmia services, and also cardiac transplantation. In addition to the core team of cardiologists and surgeons, the specialists collaborate with numerous other teams, including medical genetics, obstetrics/gynecology, and hepatology. The program is uniquely positioned to have close alignment between the flagship adult and pediatric hospitals, which share the same medical records and are in close proximity to each other.

Preventive Pediatric Cardiology Program
The Children’s Preventive Cardiology Program aims to identify and manage risk factors in children that contribute to heart disease as adults. Modifying behaviors and medically managing high cholesterol and blood pressure during childhood significantly decrease the chances of a heart attack or other cardiac-related concerns in the future. The Preventive Cardiology Program evaluates and treats children with abnormal cholesterol and hypertension. During the course of the outpatient treatment, patients and their families meet with a multidisciplinary team, including a pediatric cardiologist, a dietitian, and a nurse specially trained in blood pressure assessment.
Pulmonary Hypertension Program
The prevalence of pulmonary hypertension (PH) is increasing in the pediatric population because of better recognition and improved survival from a variety of childhood medical conditions such as congenital heart disease, prematurity, developmental lung disorders, autoimmunity, liver disease, and others. These varied disease states necessitate that diagnosing and caring for children with PH over time requires interaction between many different pediatric subspecialties. The Riley Pulmonary Hypertension Service consists of two nurses, a pulmonologist and two cardiologists to provide 24/7 call coverage as well as a dedicated inpatient rounding service and outpatient referral clinic.
The Riley Pulmonary Hypertension Program was created though the cooperation of two divisions (Pulmonology and Cardiology) within the Department of Pediatrics. Since its inception, the program has required and adhered to interdisciplinary collaboration. This concept has now blossomed such that an intimate working relationship has developed amongst several other departmental divisions including Hepatology, Neonatology, Rheumatology, and General Surgery as well as with IU Bloomington-based Epidemiology and Biostatistics.
The main vision will always be to provide the highest level of care to the patients and families served. The care this team provides is firmly grounded in established PH clinical care guidelines, but it is also individualized for best-practice decisions as well as maintaining a continuous search for emerging evidenced-based therapies through quality improvement and clinical research.
The pulmonary hypertension program has been identified nationally as a center with the clinical volume and expertise to participate in industry-sponsored clinical trials. To that end they have participated in trials evaluating the use of pulmonary hypertension therapy specifically in children. Locally, they are collaborating in research aimed at identifying pulmonary hypertension and lung function in patients with sickle cell disease, and working in conjunction with the department of epidemiology and biostatistics in Bloomington to better quantify side effects and parental burdens of pediatric pulmonary hypertension treatments.
Single Ventricle Home Monitoring Program
Interstage mortality between 1st and 2nd stages of the single ventricle palliation remains higher than anyone would like. In order to remedy that, all of the single ventricle, shunted patients, are enrolled in the Home Monitoring Program, which allows families to take their baby home, while giving them the close medical support they need. Families are trained on all equipment, medications, and feeding by a skilled team of discharge coordinators and cardiac nursing personnel prior to a mandatory 1-2 day “rooming in” prior to discharge in order to make sure the family is comfortable taking care of their baby at home. All families are sent home with a baby scale to follow daily weights, a pulse oximeter to measure oxygen levels and heart rate, and an IPad to record all of the information. Although these types of programs are becoming more popular around the country, this program was within the first to utilize iPads for the families. The medical team is thus able to see the baby’s information remotely, anytime day or night, and the data is automatically uploaded into the electronic medical record system. Along with physician support, the Home Monitoring Program is run by a dedicated nurse practitioner, who is the main contact for the family. This nurse practitioner is available via cell phone to answer the families’ questions about their baby, using her experience to triage the patients to appropriate medical care, allowing them to survive and thrive. This 24/7 access to medical professionals, trained to care for babies with single ventricle, shunted physiology, has allowed Riley Hospital for Children to have one of the lower interstage mortality statistics in the country.
Cardiac Genetics Program
The Cardiac Genetics Program at Riley Hospital for Children is a robust and comprehensive clinical cardiovascular genetics program covering all areas of cardiac genetics, including aortopathies, arrhythmias, cardiomyopathies, congenital heart disease, dyslipidemia, pulmonary hypertension, and more. The program has two full time cardiovascular geneticists supported by four dedicated genetic counselors. There are several multidisciplinary clinics in cardiology jointly staffed by cardiologists and medical geneticists as well as other subspecialists, to address the specific needs of certain subsets of patients. In addition, there are multiple weekly genetics clinics completely dedicated to patients with cardiovascular disease. The medical geneticists at Riley Hospital participate in all patient conferences and educational sessions, offering their unique perspective and enhancing the quality of the proposed medical and surgical care, as well as augmenting the education of fellows. They are readily available for consultation for clinical and research interests expressed by the pediatric cardiology staff and fellows, and are internationally renowned for their work in cardiovascular genetic disease.